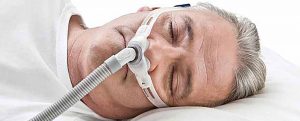
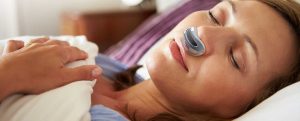
While most people take sleeping as an ordinary occurrence and don’t give a thought to it, sleeping can be a major health risk for ASA patients. Obstructive Sleep Apnea is a sleeping disorder that occurs as a result of a cyclical increase in pulmonary and systemic artery pressure.
Obstructive apneas are associated with hemodynamic changes. OSA associated with hypoxemia can cause oxygen saturation to drop even to extreme levels.
Daytime functioning of most OSA patients can go from mild to severe. These people may experience excessive daytime sleepiness (EDS) and this can b the main trigger of hypoxemia and chronic sleep disturbance. In fact, there are patients who are totally oblivious of their sleepiness and may even deny it.
Symptoms of EDS include; depression, judgment and memory problems, fatigue, personality changes, concentration difficulty and general tiredness.
OSA victims have a tendency of falling asleep at irregular times and because of this they are more vulnerable to automobile accidents and work-related accidents.
Approximately 56,000 car crashes reported by police to the National Highway Traffic Safety Administration resulted from drivers who fell asleep while driving.
There are also long term physiological effects which include increased risk during recovery and under anaesthesia and development of hypertension. OSA in children is caused by tonsillar hypertrophy and leads to behavioral challenges, reduced concentration capability, loss in weight and impaired growth.
Research is now linking attention deficit hyperactive disorder to increased cases of pediatric OSA.
OSA can also bring about Cardiac arrhythmias. In severe hypoxemia, ventricular tachycardia may frequently be observed. Normally mostly Brady arrhythmia is seen. The intensity of the OSA condition has been on the increase with new reports showing an increased risk of stroke, myocardial infarction and even death.
Diagnosing OSA
OSA can be detected by your physician through a physical exam but most importantly during the process of taking your medical history. Questions related to your sleep pattern can provide a very good lead to your condition.
Symptoms of OSA
There are 3 major symptoms of OSA. These are:
1. Chronic Loud Snoring
Patients that dont snore are unlikely to be diagnosed with OSA. However, the numbers of people who can tell if they stop breathing or if they snore are very few and therefore the best way of knowing this is to question the bed partner of other loved ones.
2. Excessive Daytime Sleepiness (EDS)
This is actually a long shot of diagnosing OSA and that many people look at as farfetched. Most people with EDS ignore the condition and unless workmates, friends, or family members complain about it, the condition might be detected too late, maybe after it causes a work-related or automobile accident.
Diagnosing OSA from this viewpoint would also include studying the body mass index, hypertension and age and should be done by an extremely sensitive person (expert).
3. Gasping Or choking in sleep
This is merely an apneic occurrence but in most cases, can’t be told by the victim. Other family members or a bed partner will therefore be relied on for this information.
There are also minor symptoms of OSA, which include:
- Restlessness
- Impotence
- Frequent nocturnal urination
- Chest and limb pain
- Dry mouth in the morning
- Gastro-esophageal reflux
- Morning headaches
- Depression and other personality discordance
- Reduced concentration ability and also poor memory
Signs of Clear Possibility Of OSA
1. Crania-Facial Abnormalities
You are more likely to be an OSA victim if there are more people in your family that have been affected. This is regardless of your alcohol consumption habits, your obesity status or even your age. In such a case OSA will result from underlying facial abnormalities or even similarity in some facial features.
2. A thick neck
A good way of predicting OSA is the size of the neck girth in both female and male people who snore. Generally a neck circumference greater than 16 inches in women and 17 inches in men is a cause for suspecting sleep apnea.
3. Cardiovascular consequences and systemic hypertension
In a series of 8 studies that incorporated 461 patients, about 55 percent of the subjects that were diagnosed with OSA also had coronary artery disease. Four other studies that took the same approach (with 166 patients) found 27% of OSA patients with hypertension. In rare cases, unexplained hypertension may also be used as a sign for OSA.
4. Obesity
People with more than 120% of the ideal body weight may be regarded as overweight or obese. Research has not found a direct link of weight to OSA as recent studies have seen more normal-weight people develop OSA. This can be attributed to pharynx anatomy or even the skull.
However, the distribution of central fat has clearly been linked to OSA. As a matter of fact, clinicians have found out that it is easier to predict OSA with the circumference of the waist than that of the neck.
The only avenue of liking obesity with OSA is linking it with strong changes of upper airway muscle changes, and damage of pharynx, tongue, and motor nerves s a result of pneumatic battering (chronic snoring).
Abnormal obesity when supine may reduce lung volumes and consequently lead to a reduction in respiratory muscle force and also influence reflexively the dimensions of the upper airway.
5. Nasopharyngeal Narrowing
Although there may be no real data to verify it, nasopharyngeal obstruction has been highly associated with OSA. It has also been seen as a common cause of OSA in children second to pharyngeal flap repair for cleft palate. The signs of nasopharyngeal include:
- A reduction in the cross-sectional area of the pharyngeal
- Increased thick and red pharyngeal mucosa
- Mandible length (Small mandibles are said to decrease the posterior airway space)
- Uvula and long soft palate
How Is Sleep Apnea Treated?
To verify an OSA diagnosis, there is a sleep study that has to be undertaken. This study is called polysomnography and will require you to stay in the laboratory overnight.
The factors that are investigated include; ventilator and airflow effort, body position, sleep staging, arterial oxygen saturation, periodic limb movements, sleep staging and electrocardiogram.
The downside of polysomnography is that it is very expensive (costing over $1000 per test) and therefore you might need insurance authorization which is normally time-consuming.
Also the result is normally not readily available and when it is, you might find it uncomfortable. Another thing is that the result of the test is highly dependent on interpretation; one cannot wholly rely on them.
Another text, called pulse oximetry, can be used to authenticate diagnosis. However, clinicians have shown concern over this test providing only moderate specificity and sensitivity when used as a stand-alone test. In a series of 12 studies that incorporated 1784 subjects who took only oximetry tests, there was an average of 65% specificity and 87% average sensitivity.
Progress on home sleep monitoring with self-contained devices that patients administer on their own and reduced channel PSG done by a technician, have not been very fruitful. Patients have found self-administering devices costly to maintain and complex to use and the simpler devices don’t meet 3rdparty reimbursement qualifications or cant be validated.
On the other hand, technician-administered home studies are more applicable for patients who can’t travel to the sleep facility for one reason or the other and maintaining them is also difficult far from the fact that they are also costly.
The latest advancement in the at-home monitoring approach is the NovaSom QSG at-home diagnostic system. This has already gotten an FDA clearance and will be offered by Sleep Solutions, Inc.
What Does A Sleep Study Reveal?
A successful sleep study will reveal the type of sleep apnea you have and how severe it is. Apnea Index (AI) is used to indicate the number of apneas per hour.
A 50%or more decrease in airflow (incomplete cessation) for greater than 10 seconds together with a 2-4% oxygen saturation drop is termedHyperpnoea.The number of hyperpnoea per hour is measured in Hyperpnoea Index (HI) the sum of HI and IA is called Apnea/Hyperpnoea Index (AHI).
Following this, it is said that the International Committee proposed and published a definition of sleep apnea in reference to AHI in the journal Sleep. According to this:
- AHI 0-5: Normal
- AHI 5-15: moderate
- AHI 15-30: Moderate
- AHI >30: Severe
Another relatively important parameter, especially in OSA victims whose cardiovascular system is compromised is the frequency and degree of oxygen de-saturations. Generally, when referring to oxygen de-saturations clinicians use mild/moderate/severe classifications.
Non-Surgical OSA Treatments
1. Continuous Positive Airway Pressure (CPAP)
The most common first therapy for moderate or severe OSA today is CPAP. CPA was officially commercialized in 1981.
Patients are prescribed a CPAP treatment after a sleep study and a CPAP titration study to know how much therapeutic level of CPAP pressure is needed to reduce or completely get rid of sleep apnea.
A patient is instructed to put on a sealed mask over their nose, (and in some instances both nose and mouth) when they sleep. This mask is connected to a blower that forces oxygen through their nasal cavity. The main role of CPAP is to increase air pressure and open the upper airway and in this way acts like a pneumatic splint.
CPAP treatment has been proven to be effective, although the compliance rate is 50-70 percent and may be higher in OSA patients whose symptoms are more severe. Most people who discontinue the use of CPAP state the inconvenience of being connected to a machine, nasal-related complaints and being unable to tolerate the mask as their major reasons.
Side Effects of CPAP
- Facial skin discomfort
- Nasal stuffiness
- Discomfort with the pressure
- Rhinitis
How to Relieve Side Effects of CPAP Treatment
- To relieve side effects, one can use nasal decongestants and steroids, humidifies and intranasal anti-cholinergic. You could also choose a more comfortable mask.
- You can improve comfort by varying the amount of pressure applied
- You can seek services of homecare companies to ensure a perfect fit and more effective equipment and they can also help you get more focus on symptom reversal.
Conclusion
CPAP treatment has proved effective in eliminating cardiopulmonary sequel and reversing daytime somnolence. If you use this treatment properly, it will enable a more rhythmic breathing. As a result, you will be able to feel better and your productivity will also increase.
Statistics have shown that OSA patients on CPAP therapy have a lower mortality rate when compared to patients who undergo other treatment modalities or those who don’t undertake any form of treatment. There continues to be improvements in machine technology and in masks which will continue to improve compliance.
Medics and patients are advised to keep follow up check-ups, especially after a month of CPAP treatment. Check-up should include;
- Assessment of patient symptoms and adherence
- Assessment of the status of a pre-existing condition like hypertension
- Assessment of the equipment status
- Adjustment of CPAP pressure in patients that have achieved noticeable loss in weight.